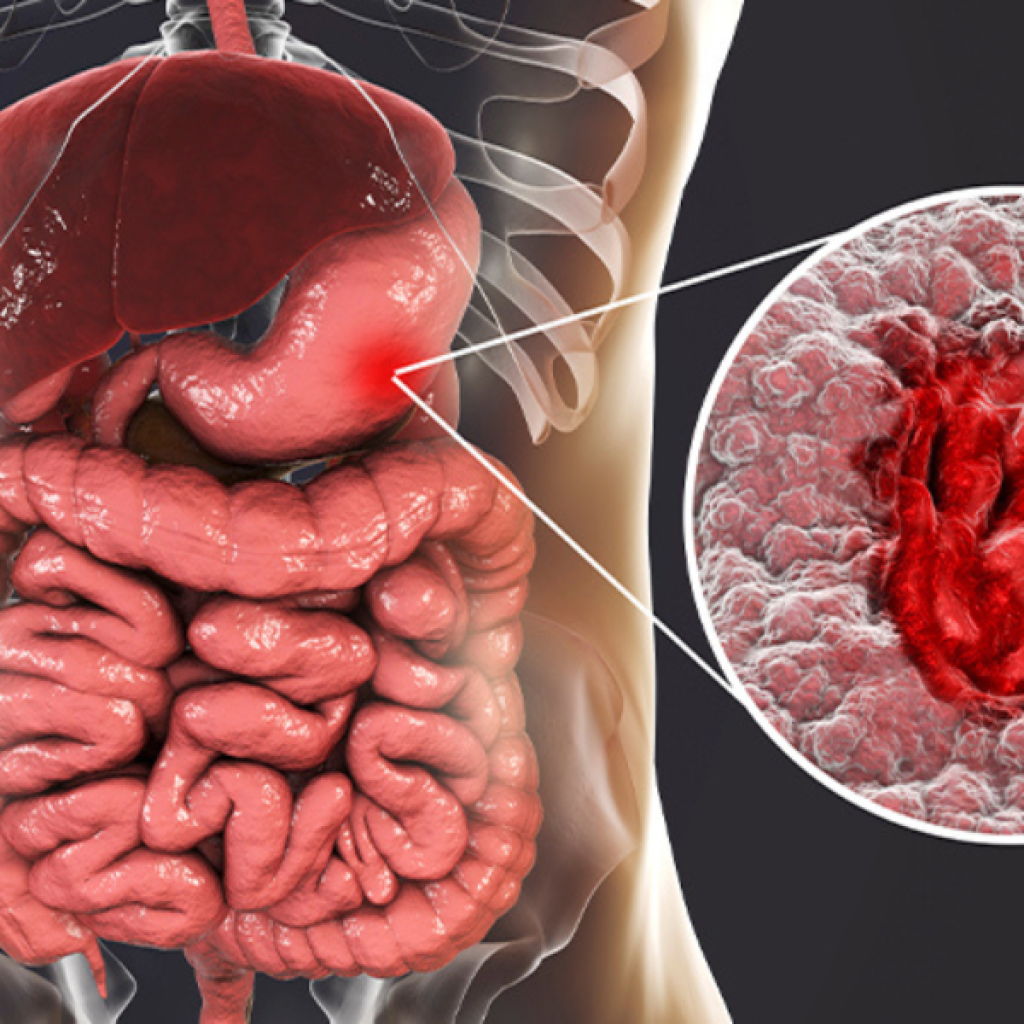
Stomach ulcers, medically termed gastric ulcers, are open sores that form on the stomach's inner lining, often causing a burning or gnawing pain in the abdomen. Once thought to be the result of stress or spicy foods, modern medicine has uncovered the true culprits behind this widespread condition, which affects approximately 6% of Americans annually and countless others globally. Understanding the causes of stomach ulcers is crucial for effective prevention and treatment, as untreated ulcers can lead to serious complications like bleeding or perforation. This article explores the primary causes of stomach ulcers, drawing on insights from medical experts and patients to provide a comprehensive look at this digestive disorder.
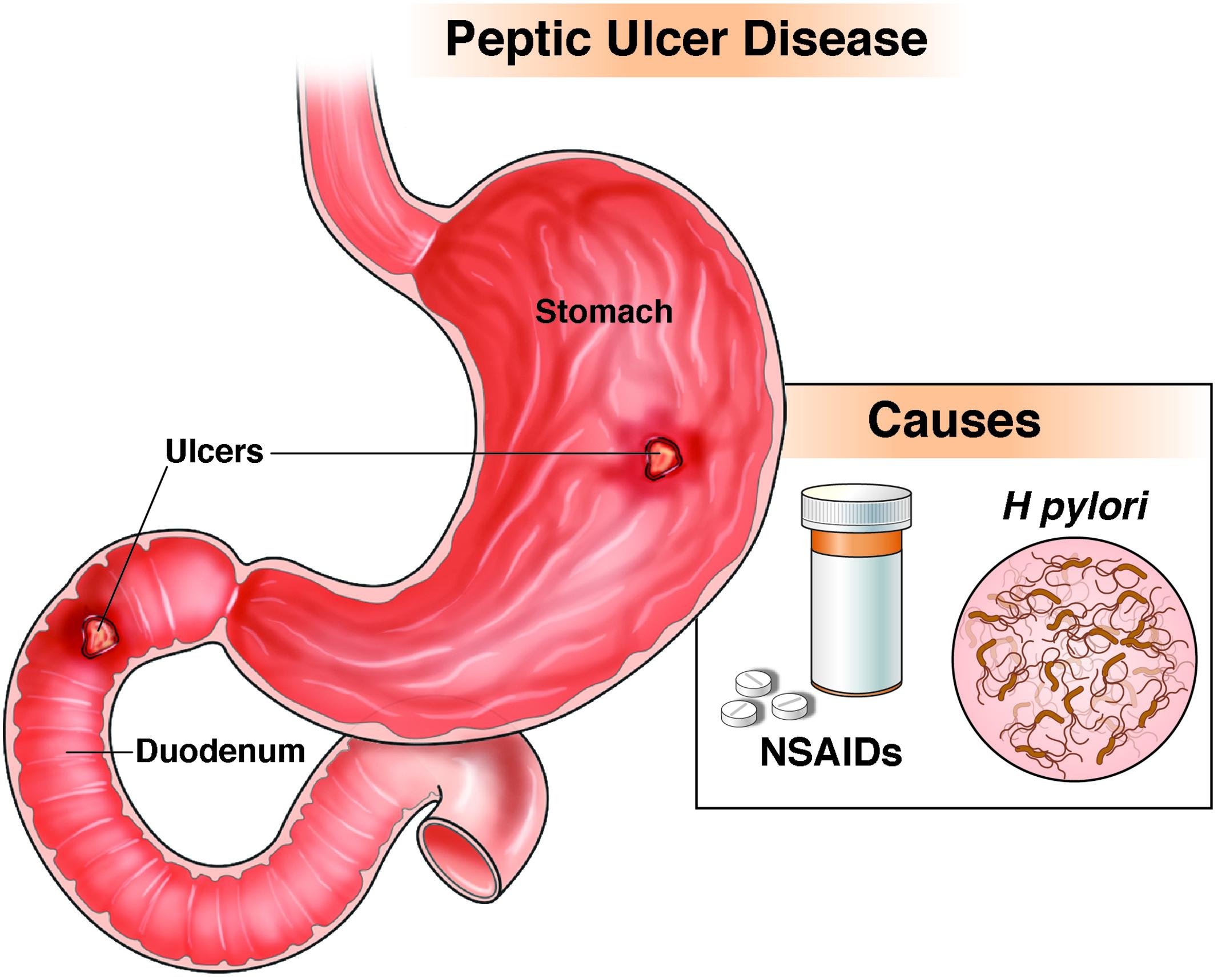
The most significant cause of stomach ulcers is infection with Helicobacter pylori (H. pylori), a spiral-shaped bacterium that resides in the stomach lining. "H. pylori is a fascinating organism," says Dr. Emily Carter, a gastroenterologist with over two decades of experience. "It thrives in the acidic environment of the stomach, which is remarkable because most bacteria can't survive there." H. pylori is present in up to half the world's population, often acquired in childhood through contact with infected saliva, vomit, or contaminated food and water. While many people with H. pylori experience no symptoms, in some cases, the bacteria disrupt the stomach's protective mucus layer, allowing acid to erode the lining and form ulcers. This infection is responsible for about 60% of gastric ulcers and up to 90% of duodenal ulcers, which occur in the small intestine just beyond the stomach.
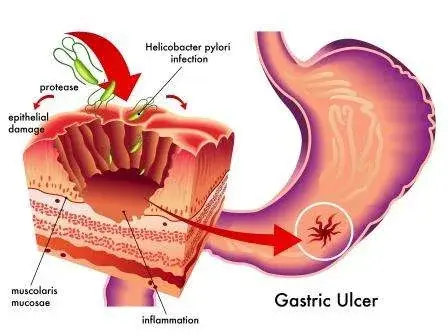
The mechanism by which H. pylori causes ulcers is complex. The bacteria produce enzymes like urease, which neutralizes stomach acid locally, creating a more hospitable environment for their survival. They also trigger inflammation by invading the stomach's surface cells, prompting the immune system to release inflammatory chemicals. "This chronic inflammation weakens the stomach lining over time," explains Dr. Carter. "It's like a slow, persistent attack that eventually creates a sore." For some individuals, this process is exacerbated by genetic factors or environmental triggers, though the exact reasons why some people develop ulcers while others do not remain under study.
The second major cause of stomach ulcers is the long-term use of nonsteroidal anti-inflammatory drugs (NSAIDs), such as ibuprofen, aspirin, and naproxen. These medications, commonly used to relieve pain and inflammation, can compromise the stomach's natural defenses. "NSAIDs inhibit the production of prostaglandins, which are crucial for maintaining the stomach's protective mucus layer," says Dr. Michael Nguyen, a pharmacologist specializing in gastrointestinal medications. "Without this barrier, the stomach lining becomes vulnerable to acid damage." This effect is particularly pronounced in individuals who take NSAIDs regularly or in high doses, such as those managing chronic conditions like arthritis. The risk is even higher when NSAIDs are combined with other medications, such as corticosteroids or selective serotonin reuptake inhibitors (SSRIs), or in individuals who also have an H. pylori infection.
For 45-year-old Sarah Mwangi, a Nairobi-based teacher, the connection between NSAIDs and ulcers became painfully clear. "I was taking ibuprofen almost daily for my back pain," she recalls. "I didn't think it could cause something as serious as an ulcer until I started feeling this intense burning in my stomach." Sarah's experience is not uncommon. Many people are unaware that over-the-counter pain relievers, often perceived as harmless, can erode the stomach lining over time. Medical professionals advise patients to take NSAIDs with food or consider alternative pain relief options, such as paracetamol, to minimize the risk.
Beyond H. pylori and NSAIDs, other less common causes contribute to stomach ulcers. Zollinger-Ellison syndrome, a rare condition characterized by tumors called gastrinomas, leads to excessive stomach acid production, which can erode the stomach lining. "This is a very uncommon cause, accounting for less than 1% of ulcers," notes Dr. Carter. "But it can be particularly challenging because the high acid levels make ulcers more persistent and harder to treat." Other rare causes include certain viral infections, Crohn's disease, and stomach cancer, which can mimic ulcer symptoms in older patients. Smoking and excessive alcohol consumption, while not direct causes, can exacerbate ulcer formation by irritating the stomach lining and increasing acid production.

Contrary to popular belief, stress and diet do not directly cause stomach ulcers, though they can worsen symptoms. "I used to think my spicy nyama choma was to blame," says James Ochieng, a 38-year-old mechanic from Kisumu who was diagnosed with an ulcer last year. "But my doctor explained it was likely the H. pylori infection I'd had for years." Research confirms that spicy foods, caffeine, and stress may aggravate existing ulcers by increasing acid production or delaying healing, but they are not primary causes. This shift in understanding has been a game-changer in gastroenterology, dispelling myths that once dominated public perception.
The interplay of risk factors can also heighten the likelihood of developing ulcers. For instance, individuals with H. pylori who also take NSAIDs are at significantly greater risk. Smoking and heavy alcohol use further amplify this risk by compromising the stomach's ability to repair itself. Blood type may also play a role; studies suggest that people with type O blood are more prone to duodenal ulcers, possibly due to differences in the stomach lining's protective mechanisms. Additionally, older adults, particularly those over 60, are more susceptible to ulcers due to age-related changes in the stomach lining and increased use of NSAIDs.
Diagnosing the cause of a stomach ulcer is critical for effective treatment. Doctors often use tests like the urea breath test, stool antigen test, or blood tests to detect H. pylori. In some cases, an endoscopy—a procedure involving a camera-equipped tube inserted into the stomach—is performed to visualize the ulcer and take tissue samples. "Endoscopy is the gold standard," says Dr. Nguyen. "It allows us to confirm the presence of an ulcer and rule out more serious conditions like stomach cancer." For Sarah, the endoscopy revealed both an H. pylori infection and damage from NSAID use, leading to a tailored treatment plan that included antibiotics and proton pump inhibitors (PPIs).
Treatment typically focuses on addressing the underlying cause. For H. pylori-related ulcers, a combination of antibiotics and PPIs is prescribed to eradicate the bacteria and reduce stomach acid, allowing the lining to heal. NSAID-induced ulcers often require stopping the medication and using PPIs or H2 receptor blockers to promote healing. Lifestyle changes, such as quitting smoking and limiting alcohol, can also support recovery. "After my diagnosis, I had to rethink my habits," says James. "Cutting out alcohol and taking my medication as prescribed made a huge difference."
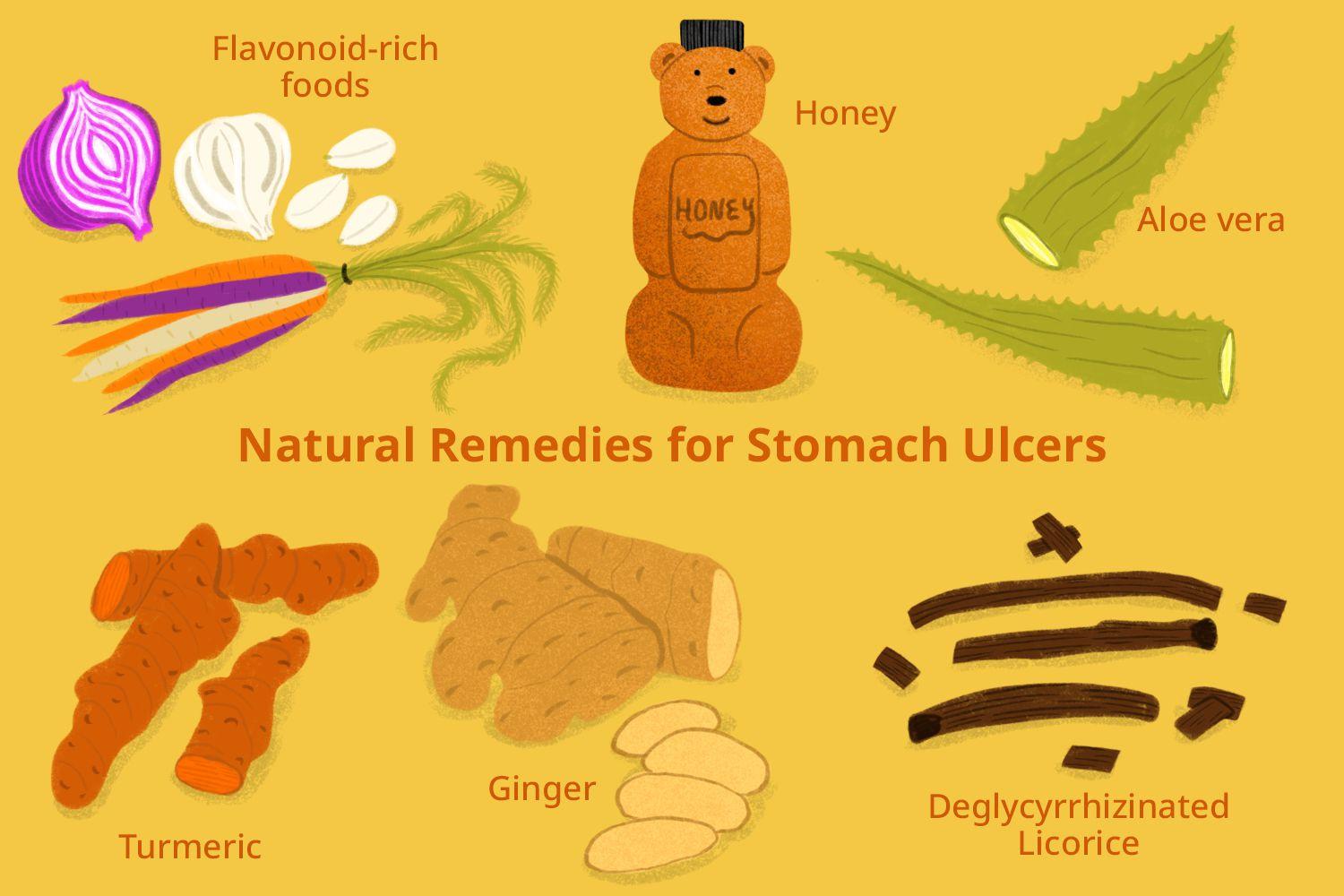
Prevention is equally important. Practicing good hygiene, such as regular handwashing, can reduce the risk of H. pylori infection. For those requiring NSAIDs, taking the lowest effective dose and using protective medications like PPIs can help. A diet rich in fruits, vegetables, and fiber may also support stomach health by reducing inflammation and supporting the gut's natural defenses. Vitamin C, found in foods like oranges and tomatoes, has shown promise in helping to eradicate H. pylori when consumed regularly.
Left untreated, stomach ulcers can lead to serious complications. Bleeding ulcers can cause anemia or life-threatening blood loss, while perforation—a hole through the stomach wall—requires emergency surgery. Obstruction, where scarring blocks the stomach's outlet, can lead to severe vomiting and malnutrition. "These complications are rare but serious," warns Dr. Carter. "That's why early diagnosis and treatment are so important."
The journey to understanding stomach ulcers reflects the evolution of medical science. Once blamed on lifestyle factors, ulcers are now recognized as primarily caused by H. pylori and NSAIDs, with rare contributions from conditions like Zollinger-Ellison syndrome. By addressing these causes and adopting preventive measures, individuals can manage and even avoid this painful condition. For patients like Sarah and James, education and treatment have been transformative, offering relief from the burning pain that once disrupted their lives. As research continues, the hope is to further refine treatments and reduce the global burden of stomach ulcers.